Associate Professor Susanna Brighenti from the Centre for Infectious Medicine (CIM) at ANA Futura, Karolinska Institutet, Sweden, is at the forefront of developing host-directed therapies (HDT) to combat tuberculosis (TB), particularly multidrug-resistant TB (MDR-TB). These therapies leverage the body’s immune system to target TB, offering a revolutionary approach to treatment.
TB remains a global health challenge, with millions of new cases each year and significant mortality rates, especially with the emergence of drug-resistant strains. MDR-TB, in particular, poses a significant threat due to limited treatment options.
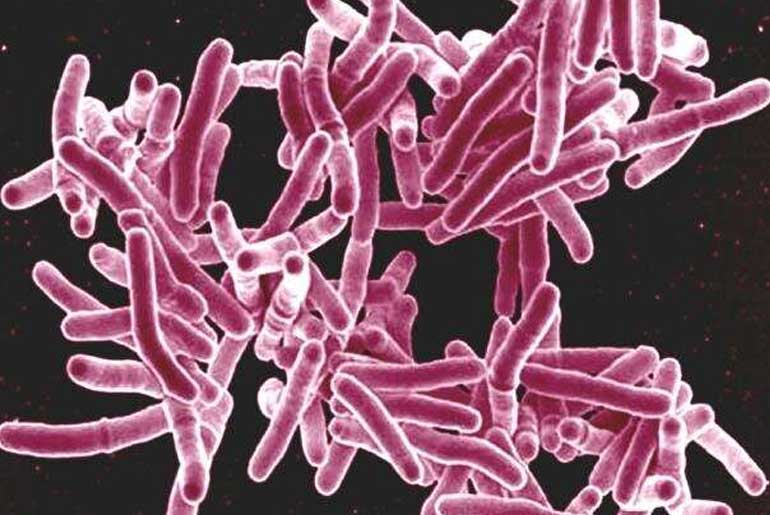
“Mycobacterium tuberculosis (Mtb) have evolved a remarkable ability to manipulate the human immune response and undermine antimicrobial effector functions in host immune cells,” explains Assoc Professor Brighenti. “While some new antimicrobial therapies are coming through, treatment with antibiotics remains an intensive and long process even for drug-susceptible forms of the disease. Importantly, mutations conferring antibiotic resistance are intrinsic properties of mycobacteria that effectively develop resistance to old as well as new groups of antibiotics, accentuating the need for adjunct treatments. Thus, new treatments are going to be absolutely vital in the battle against TB.”
HDT differs from conventional antibiotic treatments by focusing on enhancing the body’s immune responses rather than directly targeting bacterial growth. This approach involves targeting various immune pathways within infected cells to restore or induce antimicrobial functions and rebalance inflammatory responses. One example is the use of histone deacetylase (HDAC) inhibitors, which have shown promise in immune reconstitution in TB.
“These drugs can regulate transcription of genes in cells such as those in the immune system, and thus enhance the expression of proteins associated with the antibacterial host defence. We have identified several HDAC inhibitors that reduce Mtb growth inside immune cells by some 50-75%, even in the absence of antibiotics,” she explains. “That may not sound so impressive, but these immunomodulatory compounds could work well as a complement to standard therapy and exert additive or synergistic effects together with the antibiotics. This would provide the possibility to reduce the dose and treatment length required with antibiotics to improve patient outcomes.”
Assoc Professor Brighenti’s research collaboration has developed a platform for immune reconstitution in TB using small molecule compounds like HDAC inhibitors. These compounds aim to enhance the body’s immune response, potentially guarding the effect of existing antibiotics and promoting clinical recovery, especially in severe cases of TB and MDR-TB.
Instead of simply adding more antibiotics to the treatment regimen, immune-enhancing compounds could offer a complementary approach to improve patient outcomes. This personalized medicine approach recognizes that TB manifests differently in individuals and tailors treatments accordingly.
Assoc Prof Brighenti states “Implementation of immunotherapy as a complement to standard therapy has revolutionised the treatment of cancer, autoimmunity, and asthma/allergy. Similarly, our research on immune enhancement as a complement to antibiotics may become a game-changing treatment option for patients with TB that has the potential to impact clinical management and prevent spread of TB infections and drug resistance in this pivotal moment in our history when antimicrobial resistance constitutes a serious threat to human health.”
She attachs, “Short-term, approved and already available ‘off-the-shelf’ therapeutics would represent an initial logical step to implement HDTs of patients with TB. This could include for example, HDTs based on glucocorticoid treatment or cytokine neutralisation (eg. anti-IL-6, anti-1b) to reduce inflammation, while metformin, or non-steroidal anti-inflammatory drugs may also promote or rewire the immune response.”
“Long-term, more precise immunomodulatory interventions in TB such as local administration of specific HDAC inhibitors, can be tested in clinical trials with the aim to customise therapy for patients with MDR-TB. Today, several HDAC inhibitors are FDA-approved for different diseases – for example, Vorinostat, Belinostat, and Panobinostat for different cancers, Phenylbutyrate for urea cycle disorders and Givinostat for Duchenne muscular dystrophy, while the ones we have found to be most effective to reduce intracellular M. tuberculosis growth needs to be first tested in pre-clinical models for toxicity and efficacy before progressing to clinical trials.”
By presenting her research at the ESCMID Global Congress, Assoc Professor Brighenti highlights the importance of HDT in the future of TB management. These therapies offer new hope in the fight against TB, particularly in addressing the challenges posed by drug-resistant strains and improving outcomes for patients worldwide.
Disclaimer:
The information contained in this article is for educational and informational purposes only and is not intended as a health advice. We would ask you to consult a qualified professional or medical expert to gain additional knowledge before you choose to consume any product or perform any exercise.